What Is Xerophthalmia? The Causes, Symptoms, & Treatment
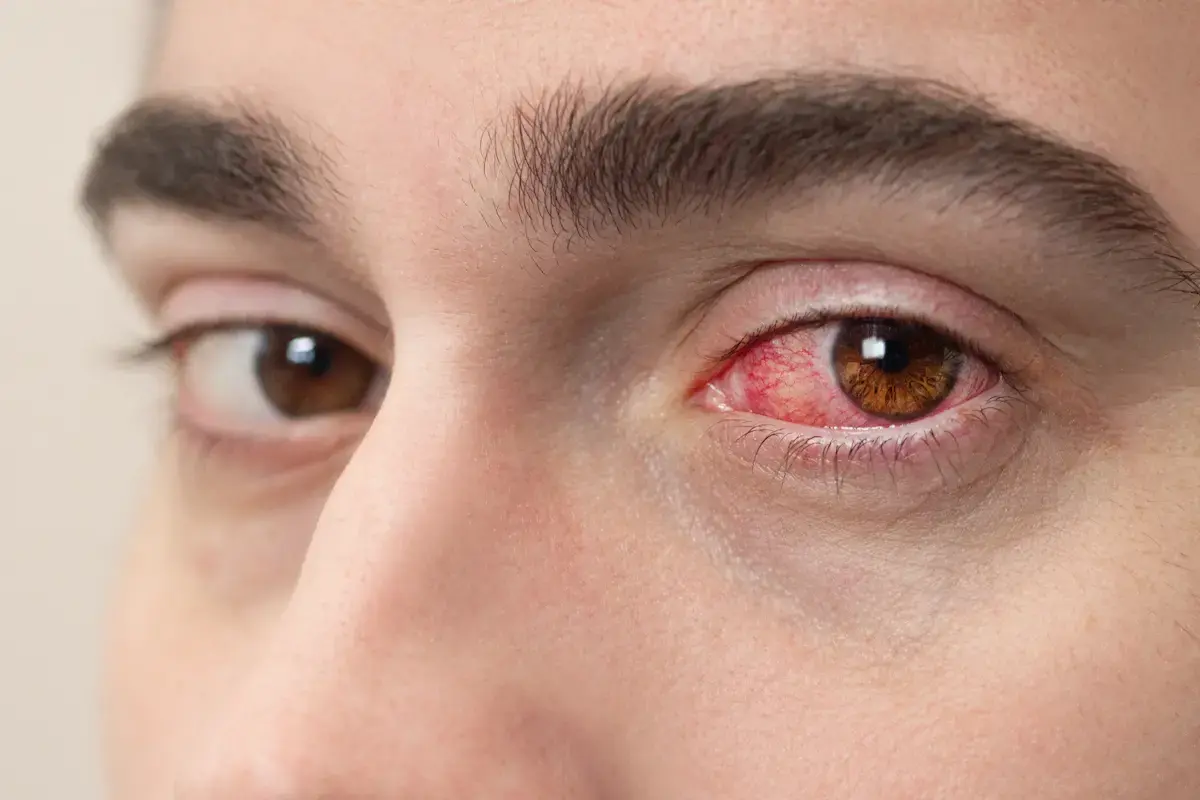
Dry eyes are often considered a minor issue, yet this condition can actually be a symptom of xerophthalmia. Xerophthalmia is a group of eye disorders caused by a vitamin A deficiency. If the body lacks vitamin A, various eye problems can arise, ranging from dry eyes to more serious damage to the cornea and retina.
Nevertheless, xerophthalmia can be prevented with fairly simple steps. To gain a deeper understanding of xerophthalmia, including its symptoms, risk factors, treatment, and prevention, read on in the following explanation!
What Is Xerophthalmia?
Xerophthalmia is a dry eye condition caused by a vitamin A deficiency. Although it is referred to as a dry eye condition, xerophthalmia also encompasses other vision disorders that can lead to a variety of problems. This condition is considered dangerous because it can progress to blindness if left untreated.
Globally, there are an estimated 350,000 cases of xerophthalmia per year. Many patients die within a year of becoming blind.
Causes of Xerophthalmia
The primary cause of xerophthalmia is vitamin A deficiency. In fact, vitamin A works to maintain corneal moisture and aids in the formation of pigments in the retina. If the levels of vitamin A are insufficient, the production and function of the eye’s protective layers can be disrupted, leading to dry eyes.
Vitamin A deficiency in xerophthalmia patients can result from two possible causes, namely:
1. Insufficient Intake
The body cannot produce vitamin A on its own. Therefore, if it does not receive sufficient vitamin A, whether from food or supplements, the risk of xerophthalmia increases. This type of deficiency is common in developing countries, where access to nutritious food remains limited.
2. Metabolic or Absorption Problems
In some people, vitamin A may be consumed, but the body cannot absorb, store, or use it effectively. This condition may be associated with certain diseases, including:
- Chronic liver disease.
- Upper gastrointestinal surgery.
- Inflammatory bowel disease.
- Pancreatic disorders (pancreatitis).
Risk Factors of Xerophthalmia
Several conditions make a person more susceptible to xerophthalmia, including:
- Childhood: Babies and children are more prone to vitamin A deficiency, especially during measles or respiratory infections. These conditions can increase the body’s need for vitamin A.
- Malnutrition: Inadequate dietary intake, particularly a vitamin A-deficient diet, can lead to vitamin A deficiency, resulting in night blindness and potentially xerophthalmia.
- Chronic diarrhea: Prolonged diarrhea can disrupt nutrient absorption, thereby increasing the risk of vitamin A deficiency.
- Liver disorders: The liver helps store vitamin A. If this organ is damaged, vitamin A reserves may be compromised.
- Certain diseases: Conditions such as pancreatitis or inflammatory bowel disease can lead to vitamin A deficiency.
- Alcoholism: Excessive alcohol consumption can lower vitamin A levels in the body.
- Poverty: Difficult access to nutritious food contributes to low vitamin A intake.
- Lack of nutrition education: A lack of understanding about the importance of vitamin A leads to an unbalanced diet.
Symptoms of Xerophthalmia
Symptoms of xerophthalmia usually appear gradually, or they do not become severe immediately. If vitamin A deficiency is not treated promptly, symptoms can progress to dryness of the eye's surface and even corneal damage. The following are common symptoms experienced by patients with xerophthalmia:
- Night blindness: Difficulty seeing in dark or low-light conditions. Patients also have trouble adapting when moving from a bright place to a dark one.
- Bitot’s spots: Grayish-white, frothy-looking spots appear on the white part of the eye. These spots are usually triangular and are characteristic of vitamin A deficiency.
- Conjunctival xerosis: The conjunctiva (the thin membrane on the white part of the eye inside the eyelid) becomes dry.
- Corneal xerosis: The cornea (the clear front layer of the eye) dries out, even though it should always remain moist. This condition can make the eye surface appear cloudy and increase the risk of corneal injury.
- Corneal ulcer: A wound or sore on the cornea. This condition requires immediate treatment because it can lead to infection, scarring, and vision impairment.
- Keratomalacia: In severe cases, the cornea may soften, become damaged, or cloud over, and may even leave scars. Keratomalacia can cause permanent blindness if not treated promptly.
- Xerophthalmic fundus: The retina experiences injury or structural changes.
Diagnosing Xerophthalmia
The doctor conducts a medical history interview by asking about the patient’s symptoms and complete health history. This history typically involves dietary patterns, social conditions, and other risk factors such as malnutrition. At this initial stage, the doctor also performs a physical examination of the eyes to look for characteristic signs of xerophthalmia, such as dry eyes, Bitot’s spots, or cornea changes.
Next, an important diagnostic procedure is a blood test. Through this test, the doctor checks the vitamin A level in the blood. If the level is below 0.70 micromoles/L, a vitamin A deficiency is likely.
In addition to blood tests, the doctor may perform visual function tests, including dark adaptometry and the night vision threshold test. Dark adaptometry measures the eye’s ability to adapt in the dark, while the night vision threshold test is used to detect night blindness.
To confirm the diagnosis, additional tests such as impression cytology and an electroretinogram (ERG) may be performed.
Treatment for Xerophthalmia Treatment
Xerophthalmia treatment aims to address vitamin A deficiency while preventing further eye damage. Some methods that can be used include:
1. Vitamin A Therapy
Vitamin A therapy is the primary treatment for xerophthalmia. High-dose vitamin A administration can help improve the condition quickly and prevent serious complications, including blindness.
According to World Health Organization recommendations, the vitamin A dose is adjusted based on the patient’s age, as follows:
- Babies <6 months: 50,000 IU.
- Ages 6–12 months: 100,000 IU.
- Children >12 months and adults: 200,000 IU.
Vitamin A is administered orally on the first day, repeated on the second day, and continued approximately two weeks later.
2. Topical Treatment
In addition to primary therapy, eye care is also necessary to maintain moisture and prevent infection. This treatment may include:
- Preservative-free eye drops or artificial tears.
- Topical antibiotics if there is a secondary bacterial infection.
In cases of corneal damage, the eye can be protected with a special shield to prevent the condition from worsening.
How to Prevent Xerophthalmia
Since xerophthalmia results from vitamin A deficiency, prevention involves consuming vitamin A-rich foods. Some recommended food sources include:
- Egg yolks.
- Beef and chicken liver.
- Cod liver oil.
- Yellow and orange vegetables, such as carrots and squash.
- Dark green vegetables, such as spinach and kale.
- Yellow and orange fruits, such as papaya and mango.
- Fortified foods and beverages, such as milk, yogurt, and cereal.
For high-risk groups, such as children and pregnant women, vitamin A intake can also be met through supplementation as recommended by a healthcare professional.
Overall, xerophthalmia is a sign of a deficiency in essential nutrients. With a balanced diet and early detection, this condition can be prevented from progressing to permanent eye damage.
If you have dry eye syndrome or risk factors for xerophthalmia, do not hesitate to consult an ophthalmologist. JEC Eye Hospitals and Clinics is a pioneer in comprehensive dry eye care. Dry Eye Services by JEC utilize a variety of sophisticated technologies for dry eye detection and examination, ranging from the Schirmer test to the TearLab® osmometer.
All our procedures are conducted in accordance with international standards and involve qualified doctors, ensuring treatment is tailored to your specific condition. JEC is ready to be your trusted partner in maintaining the quality of your vision.



 INA
INA